Your Child’s Condition
You are a partner with your child’s doctor and health care team. In order to be effective, it is important that you learn about your child’s condition. This is not a one-time activity! As your child grows and matures, their health, behavioral , and emotional needs will change and new questions will come up. In addition, new treatments and therapies may become available.
 There is a wealth of information online and your CYSHCN Regional Center will be able to guide you to resources. Your clinic, local health care system or hospital may have information or fact sheets on medical conditions. In addition, talking to other families who have a child with a similar disability or health condition may be helpful.
There is a wealth of information online and your CYSHCN Regional Center will be able to guide you to resources. Your clinic, local health care system or hospital may have information or fact sheets on medical conditions. In addition, talking to other families who have a child with a similar disability or health condition may be helpful.
Online starting points include:
- American Academy of Pediatricians Children’s Health Topics
- Medline Plus Genetics
- Kids Health Disease and Conditions
- National Center on Birth Defects and Developmental Disabilities
(Centers for Disease Control and Prevention)
There are also diagnosis-specific organizations.
Examples include:
Medical Home
 Your relationship with your primary care provider can be a “home base” which helps you think about all the needs of your child and family. This is sometimes called a Medical Home. It is a way to know what a primary care clinic can do and how you can work with your doctor.
Your relationship with your primary care provider can be a “home base” which helps you think about all the needs of your child and family. This is sometimes called a Medical Home. It is a way to know what a primary care clinic can do and how you can work with your doctor.
You know that you have a Medical Home when your primary clinic:
- knows you and helps you with your child’s special needs
- listens to you and works with you as a partner
- helps plan your child’s care and helps connect you to community resources
- offers staff reachable when you need them and accepts your insurance
- helps with other visits and talks with other doctors and caregivers who work with your child
- works with your family to transition (move) to adult health care services when your child becomes an adult
For more information on Medical Home, go to:
- National Resource Center for Patient/Family-Centered Medical Home
- Medical Home Portal Archive
- Wisconsin Medical Home Initiative
- National Alliance to Advance Adolescent Health
LEARN MORE
To learn more about a medical home and tools families can use to partner with their child’s providers to coordinate their child’s health care go to: “Coordinating Your Child’s Health Care.”
Health Care Providers
 A child’s health care should start with a primary care provider, and your insurance may require you to choose one. Your child’s primary care provider could be a:
A child’s health care should start with a primary care provider, and your insurance may require you to choose one. Your child’s primary care provider could be a:
- pediatrician – a children’s doctor
- family physician – a doctor for both children and adults
- med-peds – (Combined Internal Medicine and Pediatrics) physician
- nurse practitioner – a registered nurse who can perform examinations, deliver a diagnosis, write prescriptions and provide referrals
- physician assistant – a medical professional who can perform examinations, deliver a diagnoses, write prescriptions and provide referrals
Your child’s primary care provider will see your child for well-child visits, give immunizations and is the first one you should consult for diagnosis and treatment of health concerns and developmental delays. The primary care provider can conduct developmental screenings to check whether your child is learning and moving as other children their age usually do.
When health care needs are more complex, the primary care provider may recommend that you visit a physician who is a specialist. A specialist is a doctor who is an expert in one area of medicine (e.g., a heart doctor or cardiologist). You can find short descriptions of many medical specialists on the following web site:
To find the health care providers you need, you can ask doctors you already see, other families you may know through a support group or online, or check out:
- Your Children’s Resource Center or Well Badger Resource Center– they cannot recommend a doctor, but can share other families’ experiences and give you a list of options
- A diagnosis-specific organization such as the Down Syndrome Association of Wisconsin
( or 414-327-3729) or Spina Bifida Wisconsin (or 414-607-9061) - A “Medical Home” – What Should I Expect From My Doctor (A Family Voices of Wisconsin Fact Sheet)
- WI Department of Health Services: Finding and Choosing a Doctor
Local Public Health Departments

Your county’s local public health department may be a good resource for your family. Services vary by county, but may include immunization clinics and information on health care services. Find out what services and resources your county’s local public health department can offer you at:
CLINIC FOR THE UNINSURED OR UNDER-INSURED
Families who do not have private health insurance or public benefits (such as BadgerCare Plus or Medicaid) or do not have a regular source of health care may not have a primary care provider. There are clinics and programs in Wisconsin that see families without insurance and/or who have low income. There are many free clinics, Federally Qualified Health Centers, Rural Health Centers, and Tribal Health Centers; any of which may become your Medical Home and help you find a primary care provider. They may also be able to help you and your family explore options to better connect with health insurance coverage.
A list of clinics, services and other resources can be found at:
Oral Health
Regular visits to the dentist and good oral hygiene at home are important for all children, but may be challenging for a child with special needs.
Starting a relationship with a dentist early in your child’s life will promote good oral health and can help your dentist get to know your child.
For many families, paying for dental care is a barrier. To learn about options and find a dentist in your area, you can contact:
- Wisconsin Dental Association to learn about reduced rate dental practices who see patients who are uninsured or low income.
414-276-4520
LEARN MORE

Mental Health
“Mental health is not just the absence of mental disorders. It is defined as a state of well-being in which every individual realizes their own potential, can cope with the normal stresses of life, can work productively and fruitfully, and is able to make a contribution to their community.”
Source: Mental Health: Strengthening Our Response

When your child is struggling with their mental health, you may have questions and not know where to turn.
A first step to connecting with needed resources is to talk with your child’s primary care provider about your concerns. They can recommend further evaluation by a mental health professional, which could include a psychiatrist, psychologist, behavioral therapist or social worker.
Depending on your child’s diagnosis, therapy, or medications and/or other needs, ongoing treatment at school or in the community may be recommended.
To learn more about diagnosis, treatment and support for children mental health challenges, go to:
To connect with other families who have a child with an emotional, behavioral or mental health need and to learn about resources and support, contact:
- Wisconsin Family Ties
800-422-7145 - National Alliance on Mental Illness (NAMI) Wisconsin
800-236-2988 - Mental Health America of Wisconsin
866-948-6483 - Wisconsin Office of Children’s Mental Health
- Wisconsin Wayfinder Resource Network
877-WiscWay (877-947-2929)
Quality Health Care
While many therapy and treatment options are available, not every option is right for your child. Families should avoid options that might not be needed, could be harmful or could be a waste of money. You may want to research, talk with your primary care provider and check with your insurance coverage before you agree to some options.
Sources of information are:
When you consider therapies and treatments, you may want to ask providers questions like these:
- Does my insurance cover this?
- Are there risks to this therapy or treatment? If so, what are they?
- What is the evidence that this treatment is effective?
- How will failure of the therapy or treatment affect my child and family?
- What is the cost, time commitment and location of the therapy?
- Could I talk with another family about their experience with this treatment or therapy?
Think about the source of the information you read. Double check things you read on the Internet.

Definition
One term that you may hear when talking to your provider or learning about different therapy or treatment options is evidence-based practice (EBP).
What is Evidence-based Practice?
Evidence-based practice means using the best available research evidence to help guide health care and education services. Using the best research evidence helps providers give top-quality care that works well and is right for your child. The Institute of Medicine defines EBP as “the integration of best-researched evidence and clinical expertise with patient values.”
Therapy and Treatment
Some of the choices that may help your child are provided by health care or educational professionals. Below are examples of therapies and treatments that may be helpful.
Medications
Your child’s doctor may recommend prescription medications to treat your child’s condition. Make sure you understand what is being prescribed, including the dose, what the medication is treating and what side effects to look out for. If you are unsure, talk to your doctor and pharmacist about any drug allergies your child has, other medications your child is taking, (including vitamins and other supplements), and any special diets your child may be trying.
You can learn more about prescriptions by talking with your pharmacist and researching medications. Be sure to discuss any concerns you may have with your child’s doctor.
For information on prescription drugs:
Speech Therapy, Occupational Therapy, and Physical Therapy
Speech, occupational and physical therapies may be available through schools, medical clinics or community providers.
To learn more about each of these therapies, go to:
- Finding Your Way: Videos for Families — Outpatient Therapies
- What is speech therapy?
- What is occupational therapy?
- What is physical therapy?
School services are designed to help students learn in school. Parents may want to consider seeking additional therapies outside of the collaborative consultative services provided in public schools if they feel the needs extend beyond the school setting. To learn more about schools and collaborative consultative with speech, occupational and physical therapies:
Wisconsin Department of Public Instruction
School Based Speech Therapy
School Based Occupational Therapy
School Based Physical Therapy
Psychology and Psychiatry
Both psychologists and psychiatrists can diagnose and treat mental health issues, including emotional, behavioral and mental disorders. Psychiatrists are medical doctors and can prescribe medication; psychologists use treatments that do not involve medication.
Behavioral Therapy
Children with behavioral issues may need some type of therapy.
For general information about behavioral therapy, go to:
Children with a diagnosis of Autism Spectrum Disorder (ASD) will likely have some form of behavioral therapy recommended. A common behavioral therapy is called Applied Behavior Analysis. This therapy may be available through medical clinics and other community providers. Contact your CYSHCN Regional Center or talk to your primary care provider to find out if this or other therapy options are available in your community.
To learn more about behavioral therapy and other therapeutic options for children with ASD, go to:
What is Applied Behavior Analysis?
“Behavior analysis focuses on the principles that explain how learning takes place. Through decades of research, the field of behavior analysis has developed many techniques for increasing useful behaviors and reducing those that may cause harm or interfere with learning. Applied behavior analysis (ABA) is the use of these techniques and principles to bring about meaningful and positive change in behavior.”
Source: Applied Behavior Analysis (ABA)
Assistive Technology
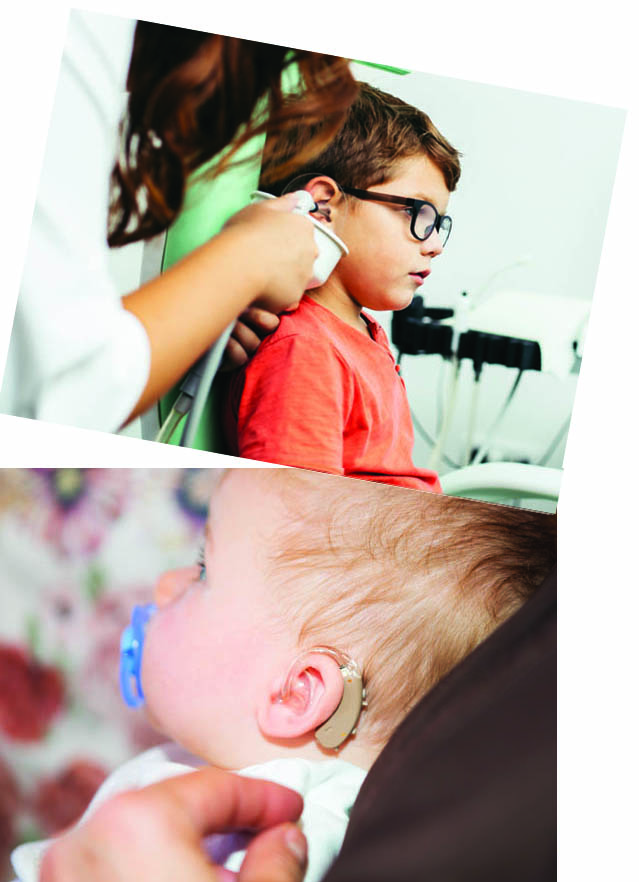 Assistive Technology (AT) is any product or device that helps people with disabilities improve their independence and quality of life. This can include anything from hearing aids to communication devices. You may be able to “borrow” a device from your Independent Living Center.
Assistive Technology (AT) is any product or device that helps people with disabilities improve their independence and quality of life. This can include anything from hearing aids to communication devices. You may be able to “borrow” a device from your Independent Living Center.
More information on Assistive Technology is available from:
- Wisconsin’s Assistive Technology Program
- Independent Living Centers in Wisconsin
- WisTech Assistive Technology Program
- Assistive Technology Lending Center (for schools)
- Wisconsin Assistive Technology Initiative (for schools)
Complementary Health Approaches
Complementary Health Approaches refer to the use of non-mainstream approaches together with conventional medical treatments. Examples include herbal and dietary supplements, massage, chiropractic and osteopathic therapies, homeopathy, deep breathing, meditation, and yoga. Talk to your primary care provider about any therapies you are considering for your child.
For more in-depth information, go to: